Significance of Minimal Residual Disease
Reading time: 3 minutes
Aishwarya Subramanian
Leukemia is a condition in which the number of white blood cells increase because of malfunctions in blood-forming tissues. White blood cells that provide immunity to the body and protect it from diseases undergo genetic alterations and mutations causing them to undergo rapid division.
When patients receive treatment for leukemia, they are closely monitored and tested at regular intervals, even once a patient has gone into remission. Why is that? Why is it so important to never miss an appointment even when a patient is in remission? The regular check-ups determine the condition of the patient and whether their cancer has progressed during their period of remission. Patients are tested and monitored to ensure that they haven’t had a relapse by closely tracking the minimal residual disease (MRD).
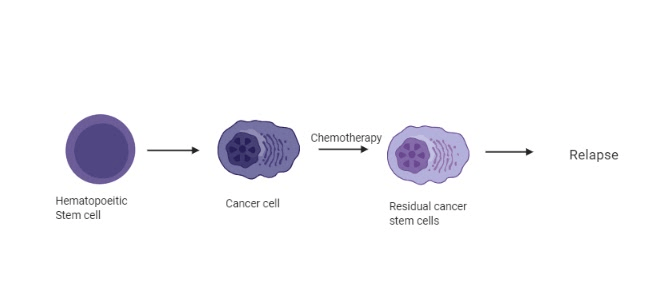
Patients at all stages of leukemia treatment are tested regularly to monitor disease progression based on the number and type of white blood cells because it helps determine the number of cancer cells that either survive or evade treatment. This is the major driver for the cancer to relapse after the patient goes into remission.
Even with newer approaches for treatment of leukemia, there is a higher rate of treatment failure. Until recently, the tests used to detect MRD were not sensitive enough. With recent research, more sensitive tests are being developed that helps to measure cancer cells in a tissue sample. The recent tests that are being developed have also been very useful for risk assessment and selection of treatment plans and provides insight on the chances of relapse and how to best avoid it. Currently the most commonly used tests are flow cytometry and PCR amplification-based methods.
Flow cytometry (a technique used to measure a certain kind of cells based on their unique physical and chemical attributes) is one of the diagnostic tools used for detection of biomarkers in leukemia. Using this method has provided an understanding of how to predict outcomes in clinical studies. Using this specific technique, detection of MRD heavily relies on identifying the different markers that are released in their environment by the cancer cells or are expressed on the surface of the cancer cells. Using these patterns of expressions a normal cell is differentiated from a leukemia cell.
PCR is a method which can be used to detect the unusual genetic alterations present in cases of leukemia and compare it with genetic make-up of a normal cell. This helps to understand the specific difference between the genetic make-up of a healthy cell versus a leukemic cell and provides a path forward to specifically target the cells.
However, even with all the data that’s been generated, studies have not had enough patients to understand enough about MRD and what kind of relationship it shows with other risk factors. More data needs to be generated to better understand this disease and use it to the advantage of developing a more effective treatment thereby, having less relapse cases.
Edited by Isabel Newsome
References:
- Minimal residual disease detection in childhood precursor B-cell acute lymphoblastic leukemia: relation to other risk factors. A children’s oncology group study- M J Borowitz, D J Pullen, J J Shuster, D Viswanatha, K Montgomery, C L Willman & B Camitta- https://doi.org/10.1038/sj.leu.2403001
- Prognostic and therapeutic implications of minimal residual disease detection in acute myeloid leukemia- https://doi.org/10.1182/blood-2011-08-363291

Leave a comment