Reading time: 5 minutes
Muhammad Ayhan Murtaza
The word phototherapy comes from two words, “photo” and “therapy” which, evidently so, means “medical treatment using light”. The word has its roots in the older Greek language, but much like this old language, cancer is by no means a newer predicament. In fact, it actually predates human evolution and is observed in other multicellular organisms too, such as fowl. Even though cancer is an archaic ailment, the proper scientific inquiry of cancer began in the last 200 years.
Virchow, the pope of medicine, was the first one to study cancers in detail. He studied what he later named leukaemia and characterised it as a blood disease. Later on, with the increase in the knowledge of cell biology, microbiology, molecular biology, molecular genetics, virology and now epigenetics, the biology of cancer was deciphered with translations into the cancer care in terms of therapy: from radiation, chemotherapy, modern-day precision therapy, and immunotherapy. Now with a more thorough understanding of the nanostructures of chemical compounds within the human body and their involvement in normal cellular physiology and how they react to different frequency light waves a new form of cancer treatment is emerging – the phototherapy! (1)
In the 1960’s, phototherapy was firstly used for retinal detachment; since then it has been used for cancer treatment too, with laser beams being used to directly kill the tumor cells. But such a use of lasers was fundamentally limited for how one aligns the laser so precisely that it only ablates the cancer cells without even raising the temperature of the surrounding tissues, as this increase in temperature would also cause significant damage to the surrounding tissues. Today, these problems are being overcome by using external agents that are photosensitive i.e. they react to light in different ways. These external photosensitive agents are administered intravenously, orally, or topically depending upon the type and exact location of the cancer and are retained in them for longer intervals of time. (2) These agents provide not only precision in treatment but can also be tracked using imaging technologies. Due to the precision and selectivity as opposed to chemotherapy (that basically annihilates every quickly dividing cells – cancerous and non-cancerous included) – and non-invasive nature as opposed to (painful) surgical options, it is a promising potential treatment of cancer. There are at least two distinct types of phototherapy that exist which differ in functioning of these photosensitive agents: photothermal therapy and photodynamic therapy.
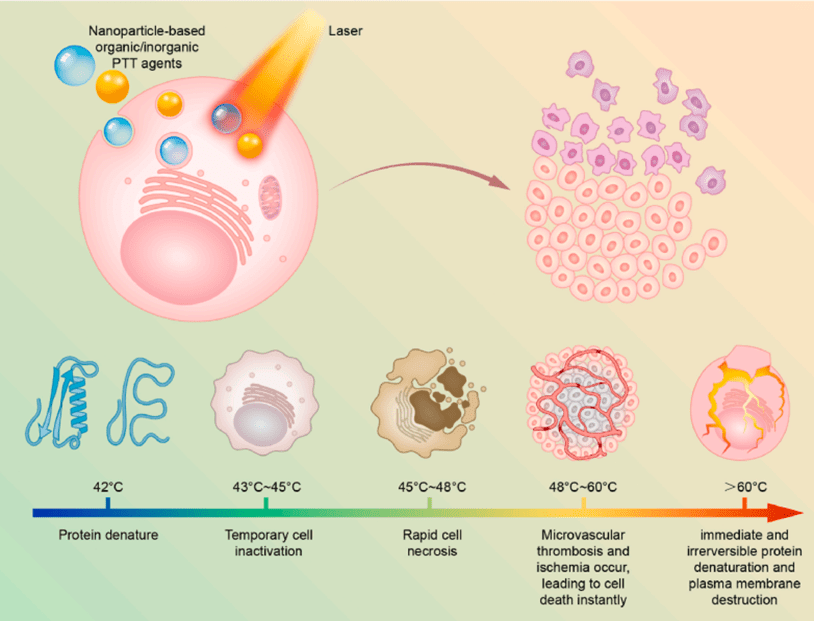
In photothermal therapy (PTT), heating the photosensitive agents that have been taken up by the cancer cells is used to destroy them in different ways at different temperatures. At increasing temperatures the photosensitive agents collide with the compounds present within the cells changing them in different ways, resulting in varied types of death of the cancer cells. Proteins, the metabolic machinery of the cell, start to disrupt first of all as they are the most sensitive to temperature. This inactivates the cell, followed by the death of the cell. When the temperature increases beyond a certain point, ischemia and ultimately plasma membrane destruction occurs. A timeline is presented in the following diagram. (2)
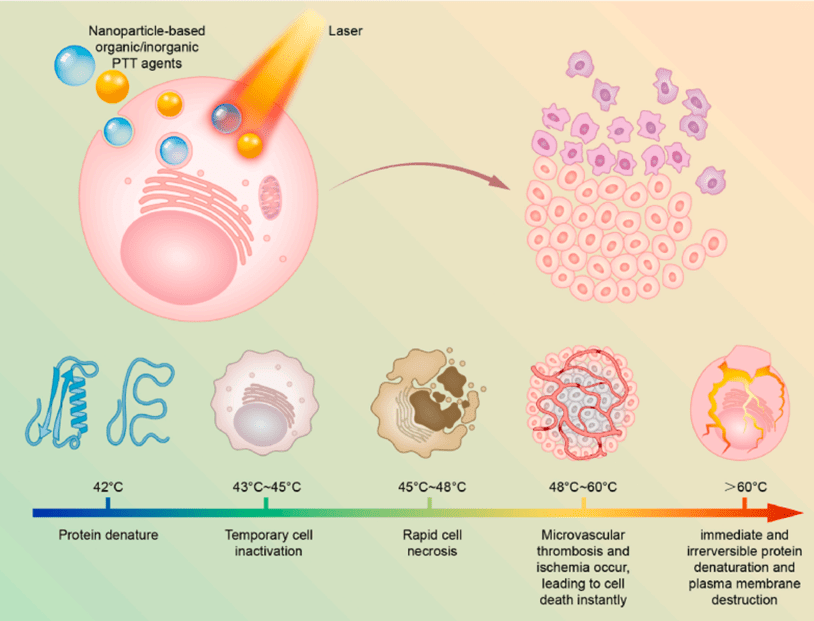
In photodynamic therapy (PDT), a photosensitizer molecule – or a metal nanoparticle – present within the cell absorbs energy when illuminated and this energised photosensitizer molecule collides with other substances present inside the cell forming unstable molecules that contain oxygen [Reactive Oxygen Species] which easily react with other molecules in a cell. (2,3)
Despite this promising potential, clinical translation of phototherapy in the last 15 years has been limited, principally due to difficulties in illumination of photosensitive agents in deep tissues. Currently, both PTT and PDT are being explored and so is their synergistic use (1). Use of chemotherapy together with these therapies would potentially inhibit any proliferation of any leftover cancer cells. Combining immunotherapy with these is also being investigated as phototherapy may be able to cause immunogenic death of the cancer cells (2).
Edited by Susan Egbert
References:
- Shi, H., & Sadler, P. J. (2020). How promising is phototherapy for cancer?. British Journal of Cancer, 123(6), 871-873.
- Xie, Z., Fan, T., An, J., Choi, W., Duo, Y., Ge, Y., … & Kim, J. S. (2020). Emerging combination strategies with phototherapy in cancer nanomedicine. Chemical Society Reviews, 49(22), 8065-8087.
- Li, J., Wang, S., Fontana, F., Tapeinos, C., Shahbazi, M. A., Han, H., & Santos, H. A. (2023). Nanoparticles-based phototherapy systems for cancer treatment: Current status and clinical potential. Bioactive Materials, 23, 471-507.

Well done Ayhan.
LikeLike