Reading time: 5 minutes
Patty Spears
Patients need more treatment options for metastatic breast cancer (MBC). MBC is when the cancer has spread from the breast to other parts of the body. Most patients with MBC stay on continuous treatment. This means that even those who live longer accumulate many toxicities (treatment costs and side effects) over time. Even with proper treatments, cancer eventually grows when it no longer responds to treatment. This leads to many changes in treatment over time. There are still unanswered questions about MBC that might affect its treatment. Specifically, we need to know more about how the cancer spreads and how best to treat it once it spreads to other parts of the body.
Definitions
Metastatic Breast Cancer (MBC)
Breast cancer that has spread beyond the breast to other parts of the body
Responds to treatment
Improvement related to treatment. The tumor shrinks or stays the same.
Molecular Subtype
A way to divided cancer (subtypes) based on whether certain genetic changes or other biomarkers are present.
Biomarker
Is there a way to treat patients with MBC with more precision? That is to say, can we find out how to give the right treatment, to the right patient, at the right time? With many new tests that look closely at cancer cells, there should be a way to use this information to guide individualized treatments. Receiving the best treatment for their cancer will allow patients to live longer and live better.
Recently a paper was published that shed light on MBC. This paper described the results of the AURORA US Retrospective Metastatic Project (Garcia-Recio, et al, 2022). This project looked at the original tumor in the breast and the metastatic tumor in other parts of the body in the same patient. Researchers looked at tumor samples previously collected and stored for future research. They also looked at treatments given to patients to understand how the treatments worked. In this project, they could look at more than one metastatic tumor from one patient.
The AURORA US study is a unique multi-institutional partnership of the Breast Cancer Research Foundation (BCRF) and the Translational Breast Cancer Research Consortium (TBCRC). AURORA US is a collaboration among many scientists, clinicians and patient advocates from 17 institutions.
About the AURORA US Retrospective Research Project
Why is this project important?
Researchers want to understand how cancer spreads and learn which cancers will respond to treatments. They also want to know which cancers will not respond to treatments, so patients will not experience toxicities from a treatment that will not work. They looked at original breast cancer tumors, metastatic tumors and clinical information from each patient. They looked at how patients were treated and if the cancer got better or worse over time. This project is important because it brings together tumor and patient information. The findings of this project may help future patients with MBC.
Which patients contributed to this project?
This project used tumor samples from patients who had MBC at diagnosis (de novo) or after treatment for early-stage breast cancer (recurrent). There were samples identified from 55 patients, which included 51 primary tumors and 102 metastatic tumors. It was important to have sets of primary and metastatic tumors from the same patient (paired samples). This study looked at 39 primary tumor samples paired with at least one (sometimes more) metastatic tumors from the same patient. Having more than one tumor from one patient allowed for the examination of cancer that has spread to different organs. There were also some samples collected at different times during their treatment.
What was done?
Usable stored samples were identified and sent to a research lab where genetic material (RNA and DNA) was isolated. The genetic material was used for several tests. (Box 1)
- RNA sequencing determined the molecular subtype of the tumors and looked at genes that may be turned on or off in the different tumor samples.
- DNA sequencing looked at changes (mutations) in the DNA of the different tumor samples.
- DNA methylation looked at modifications to the DNA that may turn genes on or off

They also collected important clinical information from each patient, including a description of how patients were treated over time. Researchers compared primary tumors (before treatment) to metastatic tumors (after treatment). They looked for changes in the cancer cell that may help us understand how cancer cells spread and how to treat it.
What was found?
There were several key findings.
- Genetic changes in the metastatic tumor led to a new treatment option in 1 of every 3 patients. In these patients, the metastatic tumor was a different subtype than the original tumor (Box 2)
- Specific changes in cancer cells suggested that an immune therapy drug may not work. A new finding showed that the amount of HLA-A on a tumor may affect which immunotherapies may or may not work.
- The number of immune cells around the metastatic tumor was different in different organs
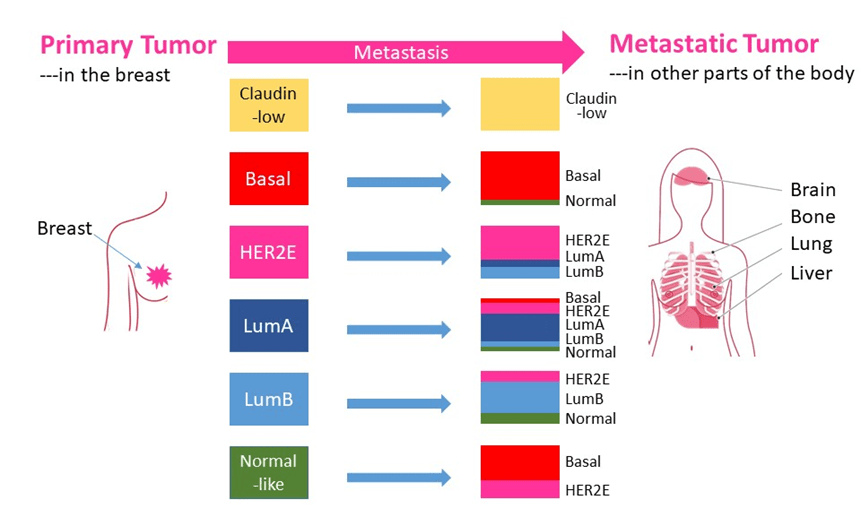
Importantly there is clinical significance to these results. Patients should have a biopsy of metastatic tumors. The information about metastatic tumors may lead to a different treatment option. This is because in 1 of 3 patients the metastatic tumor was different in some way from the primary tumor in the breast. These changes may indicate a different treatment may work against the metastatic tumor.
This project brings us closer to understanding MBC and how best to treat patients. The project also identified potential biomarkers that provide information about whether a treatment will work. It has also highlighted that MBC may behave differently in different organs.
Next steps
This project was a retrospective project, meaning it looked back at events that already took place. Retrospective projects are limited to samples and information that are already available, rather than collecting new samples. This important project is the foundation that supports the AURORA US prospective research study. A prospective study identifies patients and then follows them forward in time, collecting samples in real time. The AURORA US prospective study will enroll about 300 current patients with MBC. The focus of the prospective study is to collect and look at tumor samples, blood samples and treatment information from patients and follow their progress over time.
The findings of AURORA US may help future patients with MBC.
Edited by Ryan Ripsman
Article Referenced
Garcia-Recio, S., Hinoue, T., Wheeler, G.L. et al. Multiomics in primary and metastatic breast tumors from the AURORA US network finds microenvironment and epigenetic drivers of metastasis. Nat Cancer. 2023 Jan;4(1):128-147. doi: 10.1038/s43018-022-00491-x. Epub 2022 Dec 30. PMID: 36585450; PMCID: PMC9886551.
AURORA US Partnership
The AURORA US study is a partnership of the Breast Cancer Research Foundation (BCRF) and the Translational Breast Cancer Research Consortium (TBCRC). The study involves 17 institutions. The study is a collaboration among many scientists, clinicians and patient advocates.
Public information about AURORA US is available at auroraus.org
Clinical trial information about AURORA US Prospective Study is available at clinicaltrials.gov


Leave a comment