Taylor A. Johnson
October is the official month of breast cancer awareness. Breast cancer is one of the most common forms of cancer, especially in women. Last year alone, the American Cancer Society estimated over 300,000 new cases of breast cancer would develop in men and women, and over 41,000 would pass away from breast cancer. One of the challenges with treating breast cancer is prescribing appropriate treatment(s) based on what is triggering the cancer development.
The American Cancer Society has categorized invasive breast cancers (cancers that have grown into the breast tissue) based on 1) presence/absence of certain hormone receptors, and 2) whether they express high levels of HER2 (HER2+; human epidermal growth factor receptor 2). HER2 is a cell receptor responsible for regulating growth and division, but when overexpressed promotes cancer development by stimulating uncontrolled growth. Although HER2+ breast cancer is less common than HER2- breast cancer, it is more aggressive and carries a worse short-term prognosis.
Fortunately, there are a growing number of antibody-based therapy options for HER2+ breast cancer. Among these antibody-based therapies are Trastuzumab (brand name Herceptin), Pertuzumab (Perjeta), or Lapatinib (Tykerb), which may be given alone or in combination with other anticancer drugs. Herceptin, the most well known of these compounds, was approved in the late 1990’s and is on the World Health Organization’s list of essential medicines. Five years ago, Kadcyla, one of the newest HER2+ drugs, hit the market and generated substantial interest. Kadcyla (brand name for Trastuzumab Emtansine/Ado-Trastuzumab Emtansine/T-DM1) can be thought of as Herceptin 2.0.
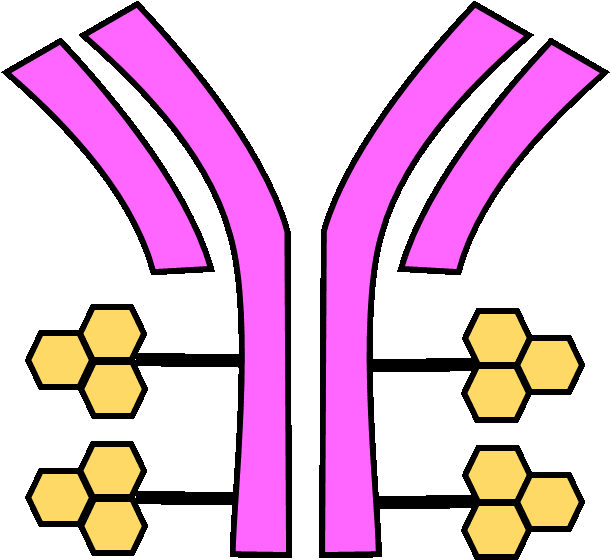
Shown in Figure 1 below, the foundation of Kadcyla is the Herceptin monoclonal antibody designed to target HER2 receptors. These antibodies have been modified to carry a cytotoxic agent known as maytansine. The idea behind Kadcyla is to use the Herceptin body to specifically deliver maytansine directly to cancer cells while also taking advantage of Herceptin’s anticancer activity. Once inside the cell, the maytansine portion (known as emtansine without the linker component) would trigger cell death by inhibiting the cancer cell’s microtubule assembly functions (1), an essential component of cell structure without which they cannot survive.
 Despite the drug’s recent availability, it has already been recommended as one standard for care. The American Society of Clinical Oncology (as of April 2018) recommends Kadcyla be used as the 2nd line of treatment for HER2+ breast cancer, and as the 3rd line of treatment if not previously administered. In addition, when Kadcyla was compared to other chemotherapeutic agents, Kadcyla was a more potent and specific therapeutic option (1).
Despite the drug’s recent availability, it has already been recommended as one standard for care. The American Society of Clinical Oncology (as of April 2018) recommends Kadcyla be used as the 2nd line of treatment for HER2+ breast cancer, and as the 3rd line of treatment if not previously administered. In addition, when Kadcyla was compared to other chemotherapeutic agents, Kadcyla was a more potent and specific therapeutic option (1).
Clinical trials have shown some interesting results when comparing patients treated with Kadcyla to those on alternative treatments. The TH3RESA trial examined several hundred patients from 22 different countries and determined that overall survival was longer in patients prescribed Kadcyla compared to the physician’s choice alternative. In addition, there were fewer Grade 3 or worse side effects in Kadcyla patients compared to other treatments (2). The EMILIA trial produced similar results, stating that patients prescribed Kadcyla had fewer Grade 3 or worse side effects compared to the Capecitabine and Lapatinib control patients (3). The MARIANNE study, on the other hand, did not view Kadcyla to be a superior treatment to the combination of Herceptin and taxanes, another class of breast cancer drugs (4). The group, however, did note that fewer Kadcyla treated patients discontinued the study due to side effects and their quality of life was better maintained; suggesting that Kadcyla may not be the stronger option, but the more tolerable option with less severe side effects.
Before you rush to your physician and demand a switch in treatment, it is very important to understand the context of these studies. The studies highlighted here (and elsewhere in literature) typically include subjects previously on one cocktail/treatment and then switched to Kadcyla, not patients who started on Kadcyla. In addition, after an initial analysis was reported, it was not uncommon to see patients cross over to the Kadcyla group (5). Therefore, a huge question regarding Kadcyla (and similarly structured treatments) is to determine which combination of treatments is best and whether Kadcyla is better early on in treatment or later on. At this time, roughly 40% of patients do not respond to Herceptin (6); further suggesting the importance of establishing treatment order and the necessity for additional study.
Lastly, it is important to note that Kadcyla and similar drugs do have some important side effects one must monitor during treatment. Herceptin, in particular, has shown to reduce heart contractility and cardiovascular function, however, that dysfunction can be reversible if properly managed (1). In addition, multiple studies have noted that Kadcyla may not have as severe of cardiovascular impairment compared to Herceptin, but it does have some notable blood-related side effects (i.e. thrombocytopenia, neutropenia) as well as the possibility of developing telangiectasia (abnormal dilation of blood vessels) (1,5).
The growing success of Kadcyla is not only excellent news for cancer patients and their families but also Roche (the company behind Kadcyla). Forbes recently reported the combined 2017 sales of Kadcyla, Perjeta, and Tecentriq (a PD-L1 targeting cancer drug), to be $3.5 billion dollars, with combined profits to double in three years. An investor update from Roche also detailed how Kadcyla sales improved by 10% over the course of 2017.
If things continue to improve, expect to hear a lot about Kadcyla in the news, magazines, and on television (cue the odd drug commercial)…
Taylor Johnson is a Biomedical Sciences Ph.D. Student in the Department of Anatomy & Cell Biology at East Carolina University; Greenville, North Carolina.
Works Discussed
1 – Johnson, T., Singla, D. 2018. Breast cancer drug trastuzumab induces cardiac toxicity: evaluation of human epidermal growth factor receptor 2 as a potential diagnostic and prognostic marker. Can. J. Physiol. Pharmacol. 96(7):647-654. doi:10.1139/cjpp-2018-0005.
2 – Krop, I., Kim, S., Martin, A., et al 2017. Trastuzumab emtansine versus treatment of physician’s choice in patients with previously treated HER2-positive metastatic breast cancer (TH3RESA): final overall survival results from a randomized open-label phase 3 trial. Lancet Oncol. 18(6):743-754. doi: 10.1016/S1470-2045(17)30313-3.
3 – Dieras, V., Miles, D., Verma, S., et al 2017. Trastuzumab emtansine versus capecitabine plus lapatinib in patients with previously treated HER2-positive advanced breast cancer (EMILIA): a descriptive analysis of final overall sturvival results from a randomized, open-label, phase 3 trial. Lancet Oncol. 18(6)732-742. doi: 10.1016/S1470-2045(17)30312-1.
4 – Perez, E., Barrios, C., Eiermann, W., et al 2017. Trastuzumab Emtansine With or Without Pertuzumab Versus Trastuzumab Plus Taxane for Human Epidermal Growth Factor Receptor 2-Positive, Advanced Breast Cancer: Primary Results From the Phase III MARIANNE Study. J. Clin. Oncol. 35(2):141-148. doi:10.1200/JCO.2016.67.4887
5 – Ricci, F., Le Tourneau, C. 2018. Trastuzumab emtansine in HER2-positive metastatic breast cancer: what is the best sequence? Chin. Clin. Concol. 7(1):3. doi: 10.21037/cco.2017.10.08
6 – Marty, M., Cognetti, F., Maraninchi, D., et al. 2005. Randomized phase II trial of the efficacy and safety of trastuzumab combined with docetaxel in patients with human epidermal growth factor receptor 2-positive metastatic breast cancer administered as first-line treatment: the M77001 study group. J. Clin. Oncol. 23:4265–4274. doi:10.1200/JCO.2005.04.173.